Fieldwork in Guinea
My research explores the postcolonial epistemologies and epidemic temporalities permeating the search for the ecological reservoir of the Ebola virus in Guinea, where the West African outbreak emerged in 2013.
Until 2013, Ebola seemed to belong to Central African forest ecosystems, where cross-species barriers are allegedly transgressed through bushmeat hunting and consuming. The West African outbreak surprised many specialists for it was the first time that the virus infected humans in the region. Yet until now, research in zoonosis epidemiology and microbiology has failed to identify the origin of the epidemic and to determine the identity of its animal reservoir, hypothetically located in some bat species.
The West African pandemic gave new fuel to concerns that the Ebola virus might be a vital threat to global biosecurity. In its wake, scientists from around the world have been scrambling to extract biological samples from the local wildlife. Those are sent to highly secure Western laboratories where analyses purport to discover and sequence emergent pathogens.
I conduct my fieldwork with the Guinean scientific assistants to such a viral surveillance project. I enquire about human-animal relations, the construction of scientific evidence and the role played by epistemologies of secrecy in the quest for the “hidden” reservoir of Ebola.
“We are told to treat animals humanely”
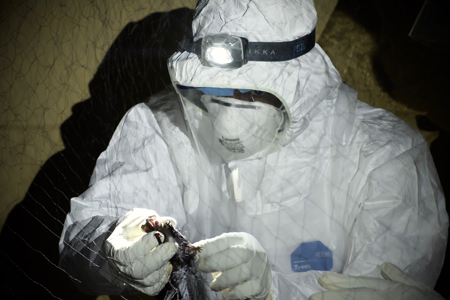
When the bats fly down into the net and become trapped, they struggle and snarl up even more tightly. A scientific agent has to disentangle the fragile jumble of hair, bones and claws, which may take several minutes. The task requires much dexterity and gentleness as one should neither tear the net nor hurt the bat. In line with contemporary Western concerns for animal welfare, the project makes bat wellbeing a priority. Yet to local fieldworkers, the animal is a rogue: it pants, squeaks and squirms to break free, its mouth open and ready to bite. The emerging concept of “One Health” invites scientific fieldworkers to literally care for the rogue as a disease sentinel that must be protected if one wishes to detect emergent threats to humans.
Through the looking shield

Virological research on lethal organisms impose a routine discipline on its agents’ bodies: the wearing of full body protective equipment. In Guinea, such a technology is materially associated with the past Ebola outbreak as all workers in the outbreak response had to don one before handling patients – outsiders often feared the masked power of those otherworldly white creatures over their lives. However, the experience of wearing a hazmat suit is rather one of encumbered bodily abilities. Sight is impaired by layers of plastic: the suit hood, the face shield, the headlamp strap, the respirator. Tiny droplets of water may fog the inner side of the face shield; the headlamp may sag. This hampers one’s capacity to communicate with coworkers and see the dangerous object of one’s focused attention. Anti-contagion technologies entail an embodied experience of vulnerability and solitude.
Needles and teeth
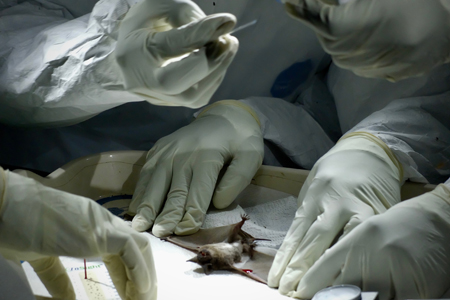
Saliva, faeces, blood and serum are sampled from up to thirty bats per night by four agents together. Their tailorized labour entangles species and materials in spaces: one person weighs the bat, one “contains” it, one samples it and one stores the samples. They wear at least two pairs of nitrile gloves, the outer pair being disinfected and changed after handling each animal. Such biosecurity precautions are meant to avert bioaccidents such as a needle prick or a bat bite through the gloves, which could potentially lead to a “spillover event,” whereby biological fluid travels across species and transmits a virus. Sampling agents intimately feel a paradoxical predicament of epidemic preparedness: if they sense that they endeavour to prevent the recurrence of another outbreak, they are also aware that their very activity could trigger one.
